Introduction
Let’s talk about something many people with diabetes worry about—but don’t always fully understand: diabetic foot syndrome. If you or someone you care for has diabetes, foot health isn’t just a “nice-to-have.” It’s a must. One small blister, one unnoticed cut, or one ignored crack in the skin can quietly snowball into a serious medical issue.
Think of your feet like the foundation of a house. When the foundation weakens, everything above it becomes unstable. Diabetic foot syndrome works the same way—starting silently and progressing fast if ignored.
What Is Diabetic Foot Syndrome?
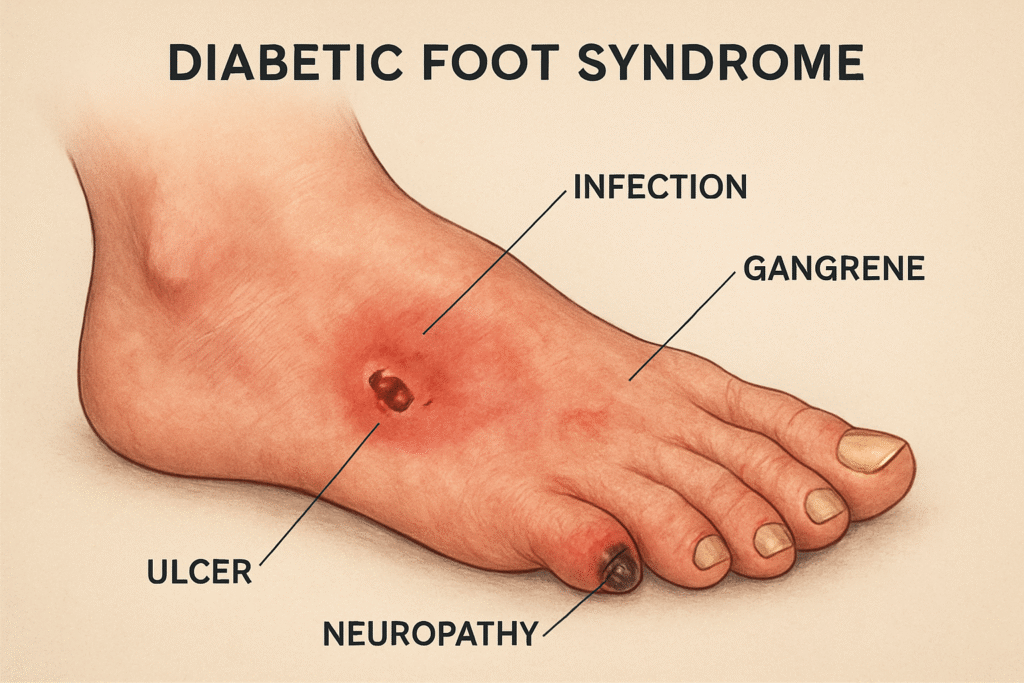
Diabetic foot syndrome (DFS) is a group of foot problems that happen because of long-term diabetes. It’s not one single condition—it’s a combination of nerve damage, poor blood circulation, and infection risk that affects the feet.
In simple terms:
- You don’t feel pain properly
- Your feet don’t heal well
- Small injuries turn serious quickly
Why Diabetic Patients Are at Higher Risk
High Blood Sugar Levels
When blood sugar stays high for years, it damages blood vessels and nerves. This damage reduces oxygen and nutrient supply to the feet, slowing healing.
Poor Blood Circulation
Reduced blood flow means wounds take longer to heal. Even a tiny cut can become a stubborn, non-healing wound.Diabetes can damage blood vessels over time, leading to reduced blood flow—especially to the legs and feet. Poor circulation slows wound healing and increases the risk of infections, ulcers, and in severe cases, amputations.
Nerve Damage
Neuropathy makes your feet numb. You may not feel pain, heat, cold, or injury. Imagine stepping on a sharp object and not realizing it—that’s how trouble starts.High blood glucose can injure nerves, causing numbness, tingling, or loss of sensation. Because of this, minor injuries may go unnoticed and worsen into serious wounds or infections.
Early Warning Signs of Diabetic Foot Syndrome
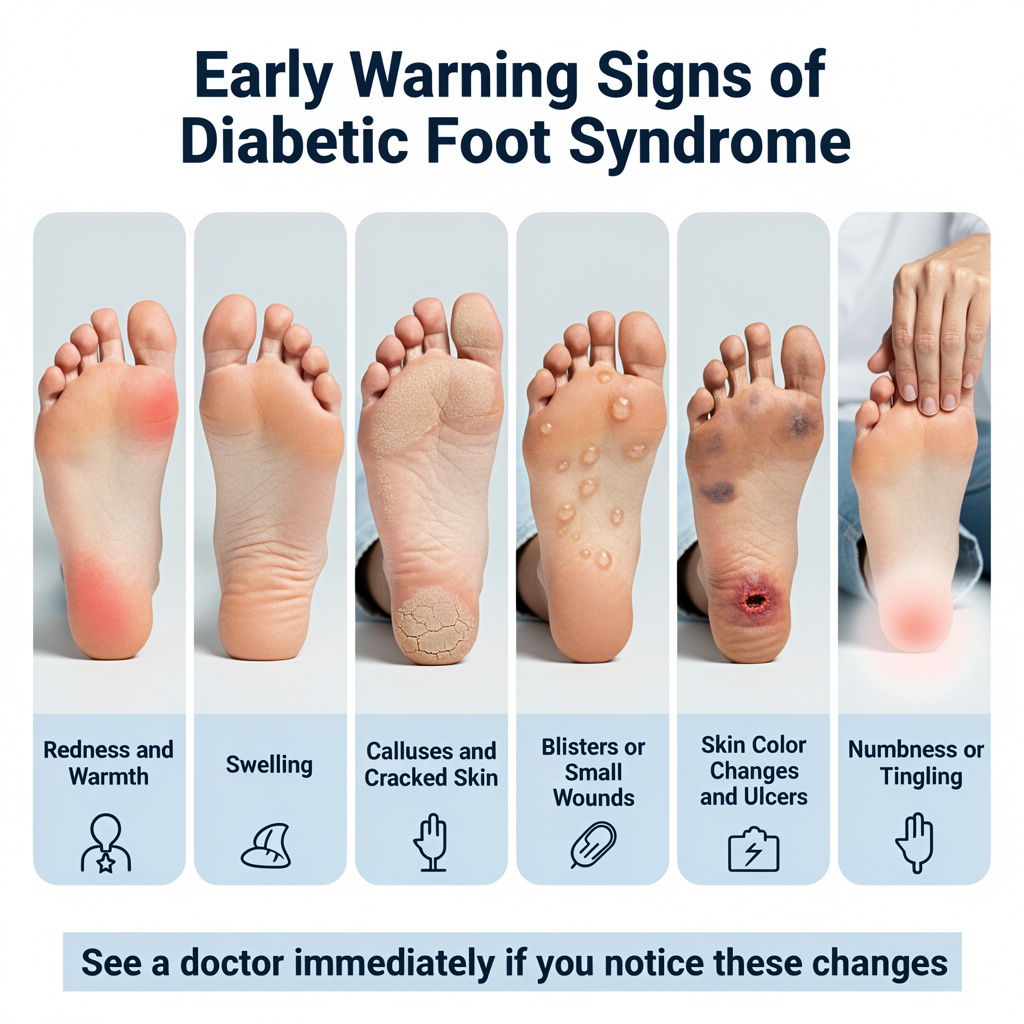
Sensory Changes
- Numbness or tingling
- Burning sensations
- Loss of temperature awareness
Skin and Nail Changes
- Dry, cracked skin
- Thick or discolored nails
- Corns and calluses
Minor Injuries That Don’t Heal
- Blisters lasting more than a few days
- Small cuts that worsen instead of healing
- Redness or swelling
Stages of Diabetic Foot Syndrome
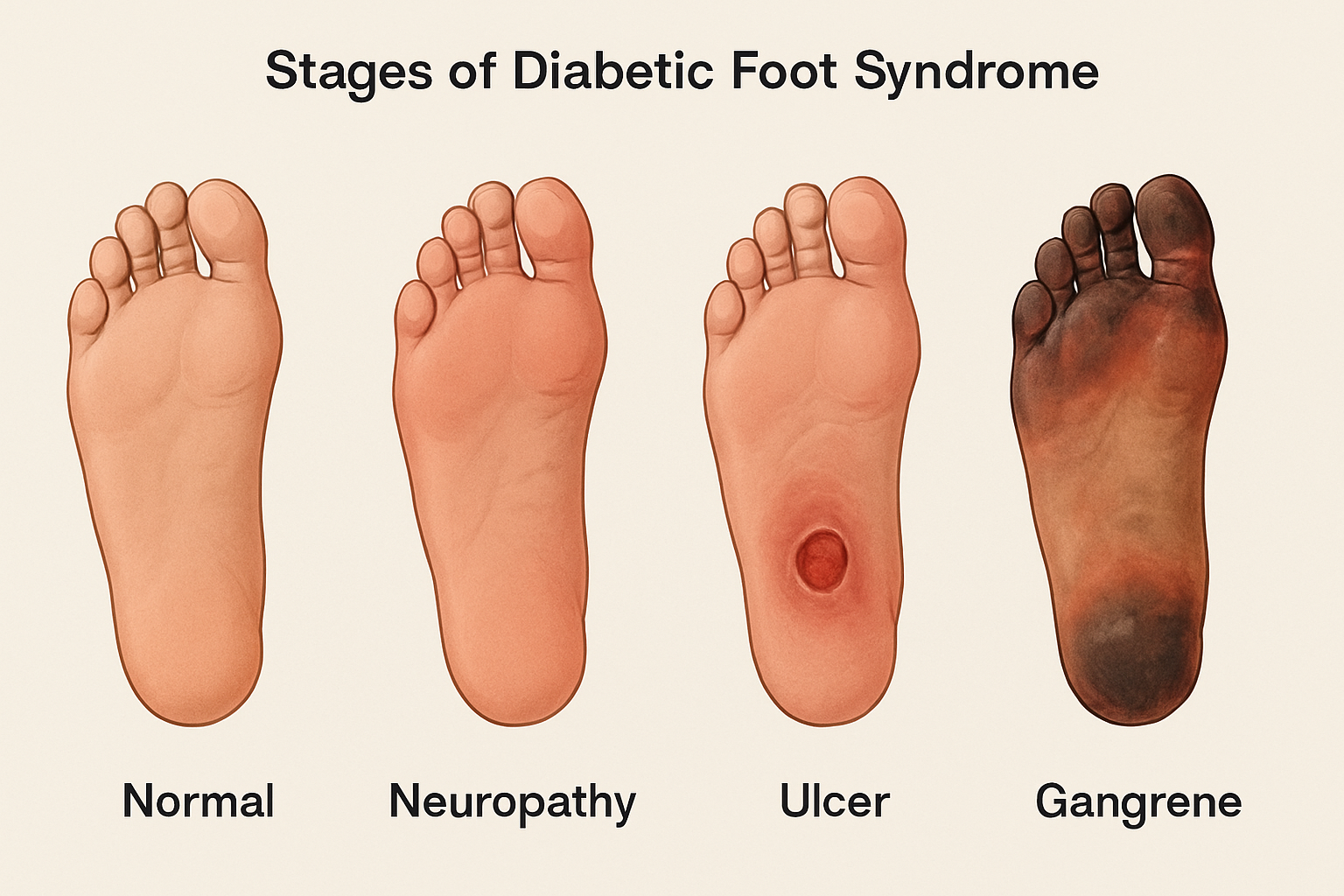
Diabetic Foot Syndrome (DFS) is one of the most serious complications of diabetes. It develops due to prolonged high blood sugar levels that damage nerves and blood vessels, increasing the risk of foot ulcers, infections, and amputations. Understanding the stages of diabetic foot syndrome is essential for early diagnosis, proper treatment, and prevention of severe outcomes.
Early Stage
- Mild numbness
- Dry skin
- Small calluses
Moderate Stage
- Open sores or ulcers
- Swelling and redness
- Mild infection
Advanced Stage
- Deep ulcers
- Severe infection
- Tissue death (gangrene)
When Complications Begin
This is where amputation risk increases. Early action can prevent reaching this stage.
Common Causes of Diabetic Foot Problems
Several factors often work together:
- Walking barefoot
- Poorly fitting shoes
- Ignoring foot hygiene
- Smoking
- Long-standing uncontrolled diabetes
Diabetic Foot Ulcers Explained
How Ulcers Develop
Pressure points + numbness + poor circulation = ulcers. A shoe rubbing the same spot daily can create a wound without you noticing.
Why They Become Dangerous
Ulcers are open doors for bacteria. Once infection sets in, it can spread fast—sometimes to the bone.
Infections in Diabetic Foot Syndrome
Infections can be:
- Superficial (skin-level)
- Deep (muscle or bone)
Signs include:
- Pus or foul smell
- Fever
- Increased pain or swelling
Diagnosis and Medical Evaluation
Physical Examination
Doctors check:
- Skin color and temperature
- Sensation
- Pulses in the feet
Imaging and Lab Tests
- X-rays to check bones
- Blood tests for infection
- Doppler tests for circulation
Early diagnosis saves limbs—and lives.
Treatment Options for Diabetic Foot Syndrome
Medical Management
- Blood sugar control
- Antibiotics
- Pain management
Wound Care
- Regular cleaning
- Debridement (removal of dead tissue)
- Specialized dressings
Surgical Options
- Drainage of infection
- Correction of deformities
- Amputation
Daily Foot Care Tips for Diabetic Patients
Small habits make a huge difference:
- Inspect feet daily
- Wash with lukewarm water
- Moisturize
- Trim nails carefully
Footwear and Lifestyle Modifications
Choosing the Right Shoes
- Soft interior
- Proper fit
- No tight spots
Habits to Avoid
- Walking barefoot
- Using heating pads on feet
- Ignoring foot pain
Prevention Strategies That Actually Work
- Keep blood sugar in range
- Quit smoking
- Regular foot checkups
- Wear protective footwear
Prevention isn’t complicated—it’s consistent.
Complications of Untreated Diabetic Foot Syndrome
Gangrene
When tissue dies due to lack of blood flow or infection.
Amputation Risks
Untreated infections may require partial or full amputation. This is why early care is critical.
Living With Diabetic Foot Syndrome
Living with DFS doesn’t mean living in fear. It means living aware. With the right care, many people manage it successfully and stay active.
When to See a Doctor
Seek help immediately if you notice:
- Any open wound
- Signs of infection
- Sudden color changes
- Increased swelling or pain
Conclusion
Diabetic foot syndrome is serious—but it’s also largely preventable. Awareness, daily care, and early medical attention can make the difference between healing and lifelong complications. Treat your feet like the valuable assets they are. After all, they carry you through life.
FAQs
1. Can diabetic foot syndrome be cured?
It can be managed effectively, but ongoing care is essential.
2. Is diabetic foot syndrome common?
Yes, especially in people with long-standing or poorly controlled diabetes.
3. Are foot ulcers always painful?
No. Many are painless due to nerve damage.
4. Can good shoes really prevent problems?
Absolutely. Proper footwear reduces pressure and injury risk.
5. How often should diabetics check their feet?
Every single day.


