Introduction
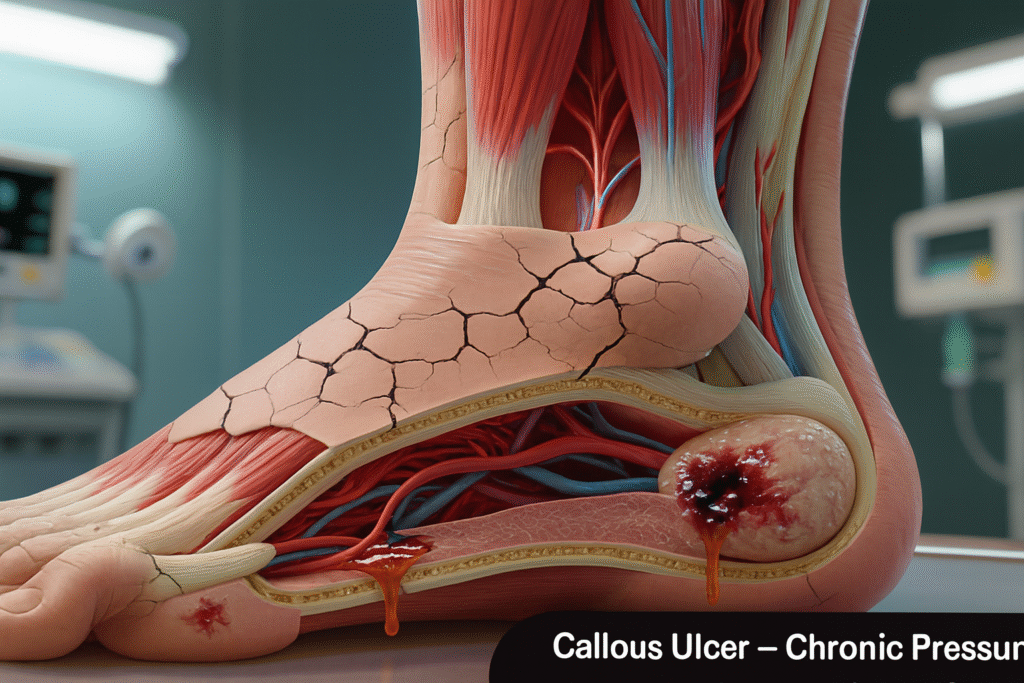
A callous ulcer is a type of skin ulcer that develops beneath or around a thickened area of skin known as a callus. A callus forms when repeated pressure, friction, or irritation causes the outer layer of skin to harden as a protective response. While this thickened skin may seem harmless at first, it can hide deeper tissue damage beneath it. Over time, the pressure trapped under the callus may cause the skin and underlying tissue to break down, eventually forming an ulcer.
Think of it like a protective shield that slowly turns into a trap. The thick callus acts as armor for the skin, but it also increases pressure on the tissues below. This pressure can restrict blood flow and damage soft tissues. As a result, a small wound forms under the callus, which may grow larger if left untreated.
Callous ulcers most commonly occur on weight-bearing areas of the feet, such as the heel, ball of the foot, or under the toes. These ulcers are especially common in individuals who experience repeated mechanical stress on their feet. Without proper treatment, the ulcer can deepen and potentially lead to infection or severe complications.
Understanding what a callous ulcer is and how it develops is the first step in preventing serious foot problems. Early detection and appropriate care can significantly reduce the risk of complications and promote faster healing.
Difference Between Callus and Callous Ulcer
Although the terms sound similar, a callus and a callous ulcer are not the same. A callus is simply a thickened layer of skin that develops due to repeated pressure or friction. Many people develop calluses on their feet or hands, especially athletes, manual workers, or individuals who walk frequently. In most cases, a callus itself is not harmful and may even serve as a natural protective barrier.
A callous ulcer, however, occurs when the pressure beneath the callus becomes excessive and leads to tissue breakdown. Imagine placing a heavy object on a cushion repeatedly; eventually, the cushion begins to wear out underneath. The same process happens with skin under a callus. The thickened skin increases pressure rather than relieving it, causing damage to deeper tissues.
Another important difference lies in symptoms. A simple callus usually appears as a yellowish or thickened patch of skin that may feel rough but does not cause severe pain. In contrast, a callous ulcer may appear as a deep wound surrounded by hard skin. Sometimes there may be drainage, redness, swelling, or signs of infection.
Recognizing the difference between these two conditions is crucial. Treating a callus early can prevent it from progressing into an ulcer, particularly for people who are at higher risk.
Why Callous Ulcers Are Common in Diabetic Patients
Role of Peripheral Neuropathy
One of the main reasons callous ulcers frequently develop in diabetic patients is a condition called peripheral neuropathy. This complication occurs when high blood sugar levels damage the nerves, particularly those in the feet and legs. When nerve damage occurs, the ability to feel pain, heat, or pressure decreases significantly.
Imagine walking on a small pebble inside your shoe. A person with normal sensation would feel the discomfort immediately and remove the pebble. However, someone with neuropathy might not feel it at all. This lack of sensation means repeated pressure or friction can continue for hours or even days without being noticed.
Peripheral neuropathy essentially removes the body’s natural warning system. Without pain as a signal, small injuries can quickly turn into serious wounds. This is why regular foot examinations and proper diabetic foot care are so important for people living with diabetes.
Impact of Poor Blood Circulation
Another key factor contributing to callous ulcers in diabetic patients is poor blood circulation, also known as peripheral arterial disease. Healthy blood flow delivers oxygen and nutrients to tissues, helping them repair damage and fight infection. When circulation is impaired, wounds heal much more slowly.
In people with diabetes, blood vessels can become narrowed or damaged due to prolonged high blood sugar levels. This reduced circulation means that even minor injuries take longer to heal. When a callus forms on a pressure point, the lack of blood flow makes it easier for underlying tissues to break down.
Poor circulation also weakens the body’s immune response. If bacteria enter the ulcer, the body may struggle to fight the infection effectively. This is why untreated callous ulcers can sometimes progress to more serious complications such as deep infections or tissue death.
Common Causes of Callous Ulcers
Continuous Pressure and Friction
The most common cause of a callous ulcer is repeated pressure and friction on the skin. Areas of the foot that bear weight during walking or standing are especially vulnerable. Each step places stress on the skin and tissues beneath the foot. Over time, this repeated pressure causes the skin to thicken as a defense mechanism.
However, the thickened callus does not always distribute pressure evenly. Instead, it may create a focal point of increased pressure on the underlying tissue. This constant force damages the tissue layer beneath the skin. Eventually, the tissue breaks down and an ulcer forms beneath the callus.
Ill-Fitting Footwear
Shoes that do not fit properly are another major contributor to callous ulcers. Tight shoes, narrow toe boxes, or high heels can create excessive pressure on specific areas of the foot. Even shoes that are slightly too small can cause repeated friction and pressure during daily activities.
When footwear consistently rubs against the skin, the body responds by forming a callus to protect the area. Over time, this protective response can become problematic. The thick callus increases pressure on the tissues below it, which can eventually lead to ulcer formation.
Footwear that lacks proper cushioning or support may also concentrate pressure on certain parts of the foot. For people with diabetes or foot deformities, choosing the right shoes becomes even more critical to prevent ulcers.
Lack of Foot Care in Diabetes
Proper foot care is essential for individuals with diabetes. Unfortunately, many people underestimate the importance of daily foot inspections and hygiene. Small cuts, blisters, or calluses may go unnoticed and untreated.
When calluses are not trimmed or managed properly, they continue to grow thicker. The increased pressure beneath the callus can damage tissues and lead to ulcer formation. In some cases, individuals attempt to remove calluses themselves using sharp tools, which can worsen the injury.
Regular foot examinations by healthcare professionals, along with proper hygiene and moisturizing, can help prevent calluses from progressing into ulcers.
Symptoms and Early Warning Signs
Physical Signs to Watch
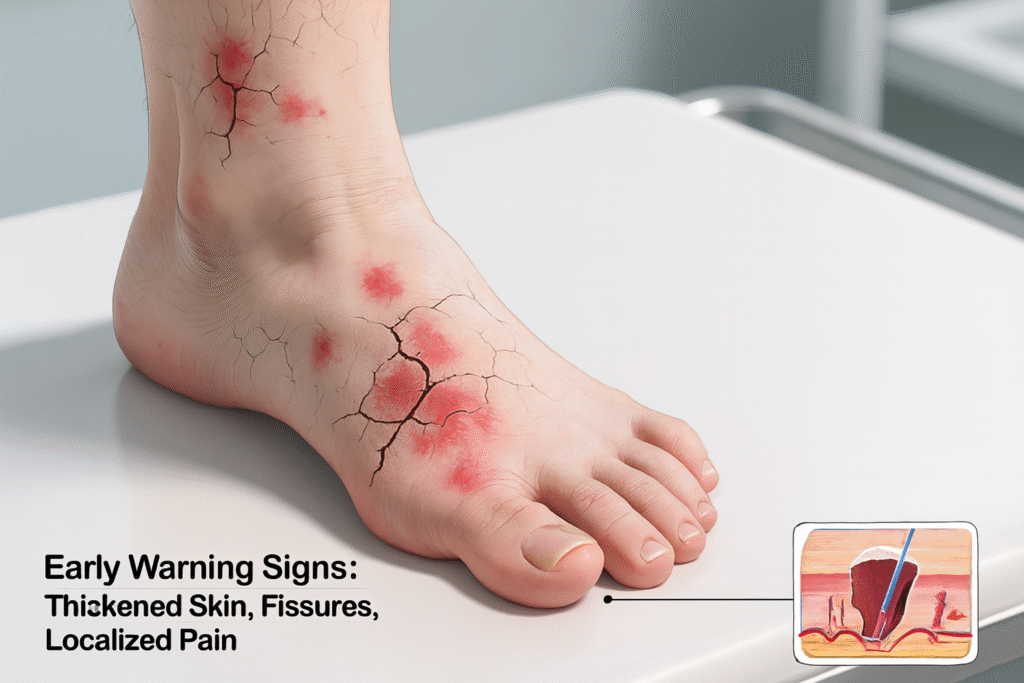
Recognizing the early symptoms of a callous ulcer can prevent serious complications. One of the first signs is the presence of thick, hardened skin on the foot, usually in areas that experience frequent pressure. The callus may appear yellowish or gray and feel rough to the touch.
As the condition progresses, a small wound may develop beneath the callus. This wound might appear as a red or dark spot surrounded by hardened skin. In some cases, the area may produce fluid or discharge, indicating infection.
Swelling, warmth, and redness around the wound are additional warning signs that should not be ignored. These symptoms often indicate that the body is responding to tissue damage or infection.
When Pain May Not Be Present
One of the most challenging aspects of callous ulcers is that they may not cause pain, especially in individuals with diabetic neuropathy. Because nerve damage reduces sensation, a person may continue walking on the affected foot without realizing that an ulcer has formed.
This lack of pain can delay diagnosis and treatment. By the time the ulcer is discovered, it may already be deep or infected. This is why healthcare providers strongly recommend daily foot checks for individuals with diabetes.
Looking for visual signs such as skin discoloration, swelling, or drainage can help detect ulcers early, even when pain is absent.
Diagnosis of Callous Ulcers
Clinical Examination
Diagnosing a callous ulcer usually begins with a clinical examination performed by a healthcare professional. The doctor carefully inspects the foot, paying close attention to areas with thickened skin or abnormal pressure points. During the examination, the callus may be trimmed to reveal the underlying ulcer.
Healthcare providers also check for signs of infection, such as redness, warmth, swelling, or drainage. They may assess the depth and size of the ulcer to determine its severity. Another important part of the examination involves evaluating foot sensation using specialized tools to detect neuropathy.
Diagnostic Tests
In some cases, additional tests are needed to evaluate the condition more thoroughly. Imaging tests such as X-rays may be used to check whether the infection has spread to the bones. Blood tests can help identify systemic infections or uncontrolled blood sugar levels.
Doctors may also perform vascular tests to measure blood flow in the legs and feet. These tests help determine whether poor circulation is contributing to the ulcer.
Accurate diagnosis ensures that the treatment plan addresses the underlying causes and prevents further complications.
Treatment Options for Callous Ulcers
Debridement and Wound Care
The first step in treating a callous ulcer is often debridement, a procedure that removes the thick callus and dead tissue surrounding the wound. Removing this tissue reduces pressure and allows the ulcer to heal more effectively.
After debridement, the wound is cleaned and covered with a sterile dressing. Proper wound care helps protect the ulcer from infection and promotes healing.
Medications and Infection Control
If the ulcer becomes infected, doctors may prescribe antibiotics to eliminate the bacteria causing the infection. Topical medications may also be applied to the wound to prevent microbial growth.
Controlling blood sugar levels is equally important for individuals with diabetes. High glucose levels slow the healing process and increase the risk of infection.
Advanced Treatment Approaches
In more severe cases, advanced treatments may be required. These may include specialized wound dressings, skin grafts, or pressure-relieving devices such as off-loading shoes. Some patients benefit from negative pressure wound therapy, which uses controlled suction to promote healing.
Early and appropriate treatment significantly improves recovery outcomes and reduces the risk of complications.
Prevention Strategies
Foot Care Routine
Preventing callous ulcers begins with a consistent daily foot care routine. Washing the feet with mild soap, drying them carefully, and moisturizing the skin can help maintain healthy skin integrity. Regular inspection of the feet allows individuals to detect changes early.
Choosing the Right Footwear
Proper footwear plays a critical role in prevention. Shoes should provide adequate cushioning, support, and space for the toes. Custom orthotics may also help distribute pressure evenly across the foot.
When combined with regular medical checkups and proper diabetes management, these preventive measures can significantly reduce the risk of callous ulcers.
Conclusion
Callous ulcers are more than just a minor foot problem. They represent a serious condition that can develop when pressure and friction cause tissue damage beneath a callus. Although they often occur in individuals with diabetes, anyone experiencing repeated pressure on the feet can develop them.
Early detection, proper footwear, and regular foot care are essential for preventing ulcers from forming. When an ulcer does develop, prompt medical treatment can prevent complications and promote faster healing. By understanding the causes, symptoms, and treatment options, individuals can take proactive steps to protect their foot health and maintain an active lifestyle.
FAQs
1. What is the main cause of a callous ulcer?
The primary cause is repeated pressure and friction on the skin, especially in weight-bearing areas of the foot.
2. Are callous ulcers common in diabetes?
Yes, people with diabetes are at higher risk due to nerve damage and reduced blood circulation.
3. Can callous ulcers heal on their own?
Small ulcers may improve with proper care, but medical treatment is usually required to prevent infection and complications.
4. How can I prevent callous ulcers?
Regular foot care, proper footwear, and routine medical checkups can significantly reduce the risk.
5. When should I see a doctor for a callous ulcer?
If you notice a wound, redness, swelling, or drainage around a callus, you should seek medical attention immediately.


