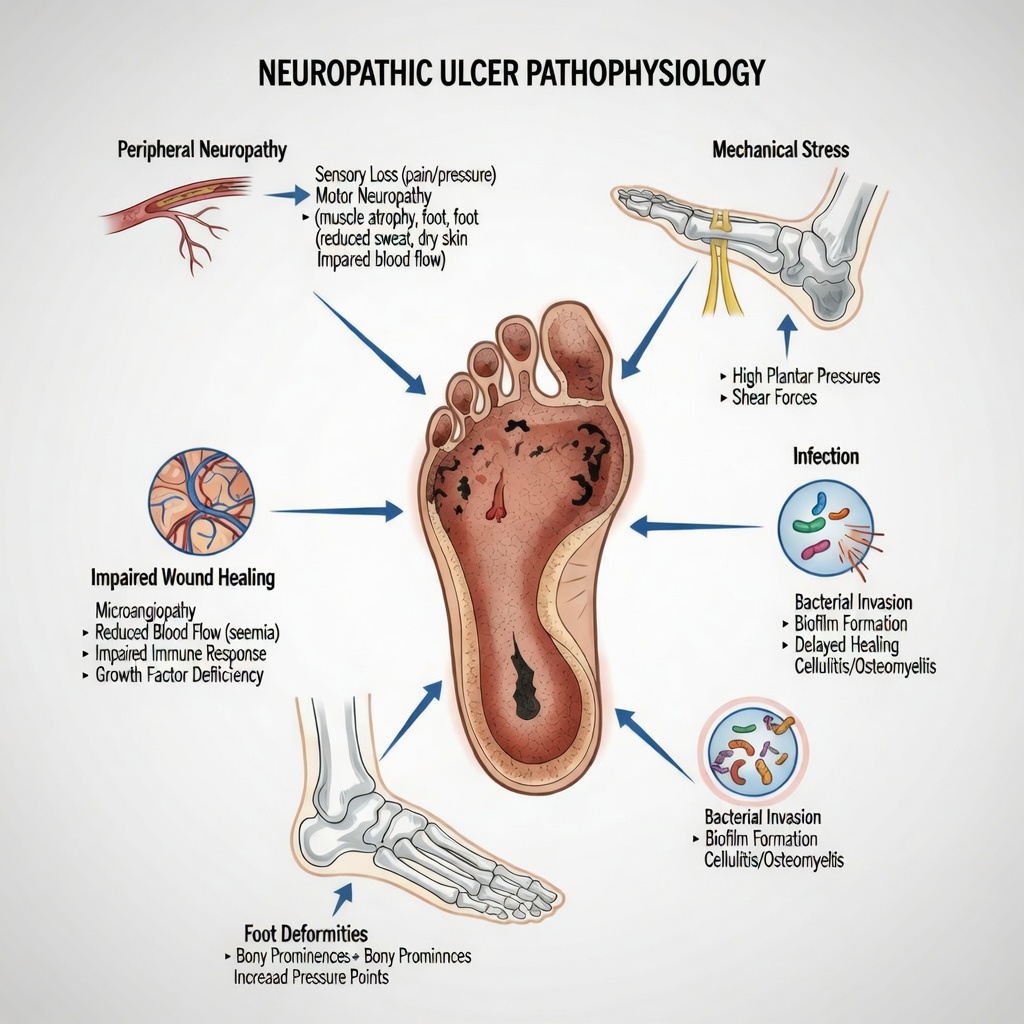
Introduction
Neuropathic ulcers are one of those silent problems that sneak up on patients without much warning. They don’t usually scream in pain or show dramatic early signs. Instead, they quietly develop, often going unnoticed until they become serious. Understanding neuropathic ulcer pathophysiology is the key to stopping these wounds before they spiral into infections, amputations, or lifelong disability.
What Is a Neuropathic Ulcer?
A neuropathic ulcer is a chronic wound that develops due to nerve damage, most commonly affecting the feet. Because nerves lose their ability to send pain signals, injuries go unnoticed. Imagine walking with a stone in your shoe all day but never feeling it—eventually, damage is inevitable.
Why Understanding Pathophysiology Matters
Knowing how and why these ulcers form helps clinicians and patients focus on prevention, early detection, and targeted treatment. Pathophysiology is the story behind the wound—and it explains everything from pressure buildup to delayed healing.
Basics of Peripheral Neuropathy
Definition of Peripheral Neuropathy
Peripheral neuropathy refers to damage to the peripheral nerves responsible for sensation, movement, and autonomic functions. When these nerves malfunction, the foot becomes vulnerable to repeated injury.
Common Causes of Neuropathy
Diabetes Mellitus
Diabetes is the leading cause. Chronic high blood sugar damages nerves and small blood vessels, creating the perfect storm for ulcer development.
Alcohol-Induced Neuropathy
Long-term alcohol use deprives nerves of essential nutrients, weakening their function over time.
Vitamin Deficiencies
Deficiencies in B vitamins, especially B12, impair nerve repair and conduction.
Types of Neuropathy
Neuropathic ulcers don’t occur due to a single type of nerve damage. They are usually the result of multiple neuropathic processes working together.
Sensory Neuropathy
This is the most important contributor. Sensory neuropathy causes loss of pain, pressure, and temperature sensation. When pain disappears, injuries go unnoticed.
Motor Neuropathy
Motor neuropathy weakens muscles and causes imbalance between flexors and extensors. Over time, this leads to deformities like claw toes or high arches
Autonomic Neuropathy
Definition of Neuropathic Ulcer
Autonomic nerve damage reduces sweating and alters blood flow. The skin becomes dry, cracked, and fragile—perfect conditions for breakdown.
A neuropathic ulcer is a chronic, non-healing wound that develops due to loss of protective sensation and repeated mechanical stress, usually over pressure points.
These ulcers are typically:
- Painless
- Surrounded by callus
- Located on weight-bearing areas
- Slow to heal
How Neuropathy Leads to Ulcer Formation
Loss of Protective Sensation
Pain is the body’s alarm system. When it’s gone, burns, cuts, and pressure injuries happen without warning.
Repetitive Microtrauma
Small, repeated injuries—like friction from shoes—build up over time. Without rest or awareness, tissue breaks down.
Pressure Points and Callus Formation
Excess pressure leads to thick calluses. Underneath these calluses, tissue hemorrhage and necrosis begin, eventually opening into ulcers.
Role of Sensory Neuropathy
Pain Insensitivity and Injury
Patients often say, “I didn’t feel anything.” That’s the danger. Sharp objects, heat, or tight shoes can damage skin without triggering pain.
Delayed Recognition of Wounds
Without symptoms, wounds grow deeper and wider before anyone notices, increasing complications.
Role of Motor Neuropathy
Muscle Imbalance and Foot Deformities
Motor nerve damage weakens intrinsic foot muscles. This leads to claw toes, high arches, and prominent metatarsal heads.
Abnormal Gait and Pressure Redistribution
Walking patterns change, concentrating pressure on specific areas—prime locations for ulcer formation.
Role of Autonomic Neuropathy
Reduced Sweat and Dry Skin
Autonomic dysfunction reduces sweating, causing dry, cracked skin that breaks easily.
Skin Cracks and Entry Points for Infection
These cracks act like open doors, allowing bacteria to enter and colonize deeper tissues.
Microvascular Dysfunction
Although major blood vessels may be intact, neuropathy affects microcirculation.
This results in:
- Reduced oxygen delivery
- Impaired nutrient supply
- Delayed waste removal
Healing becomes inefficient even when blood flow appears “normal.”
Biomechanical Factors
High Plantar Pressure
Increased pressure under the foot—especially at the ball and heel—compresses tissues, reducing blood flow and causing breakdown.
Limited Joint Mobility
Stiff joints increase stress on soft tissues, accelerating skin damage.
Inflammatory Pathways in Ulcer Development
Chronic Low-Grade Inflammation
Neuropathy creates a persistent inflammatory state that weakens tissue repair mechanisms.
Impaired Cytokine Response
The body struggles to coordinate inflammation and healing, leading to chronic non-healing wounds.
Inflammation and Impaired Wound Healing
Neuropathy alters the inflammatory response:
- Prolonged inflammation
- Reduced growth factor activity
- Impaired collagen synthesis
Role of Infection in Neuropathic Ulcers
Bacterial Colonization
Open ulcers quickly attract bacteria, especially in warm, moist environments like shoes.
Biofilm Formation
Bacteria form protective biofilms, making infections stubborn and resistant to treatment.
Common Sites of Neuropathic Ulcers
Neuropathic ulcers most often develop at:
- Plantar surface of the foot
- Metatarsal heads
- Heel
- Tips of toes
Risk Factors That Accelerate Ulcer Formation
Poor Glycemic Control
High blood sugar worsens nerve damage and impairs immunity.
Inappropriate Footwear
Tight, rigid shoes create friction and pressure points.
Previous Ulcer History
Once an ulcer occurs, recurrence risk skyrockets.
Difference Between Neuropathic and Ischemic Ulcers
Pain, Location, and Appearance
Neuropathic ulcers are usually painless and occur on pressure points, while ischemic ulcers are painful and appear on the edges of the foot.
Blood Supply Differences
Neuropathic ulcers have relatively preserved blood flow, unlike ischemic ulcers caused by arterial disease.
Pathophysiological Cascade Explained Step-by-Step
Let’s simplify the cascade:
- Neuropathy develops
- Sensation is lost
- Pressure goes unnoticed
- Skin dries and cracks
- Deformities increase stress
- Callus forms
- Tissue breaks down
- Ulcer develops
- Healing is impaired
Complications of Untreated Neuropathic Ulcers
If left untreated, neuropathic ulcers can lead to:
- Infection
- Osteomyelitis
- Gangrene
- Amputation
- Reduced quality of life
Early understanding prevents late disasters.
Clinical Implications of Pathophysiology
Knowing the pathophysiology helps clinicians:
- Focus on pressure offloading
- Address callus formation
- Improve skin care
- Educate patients effectively
Treatment without understanding the cause is incomplete.
Conclusion
Neuropathic ulcer pathophysiology is a complex interplay of nerve damage, pressure, microvascular dysfunction, and impaired healing. The real danger lies in silence—ulcers form without pain, warning, or drama. But the good news? With awareness, early intervention, and preventive care, most neuropathic ulcers are avoidable. Understanding the “why” behind these wounds empowers patients and clinicians to protect feet, preserve mobility, and prevent life-altering complications.
FAQs
1. Why are neuropathic ulcers painless?
Because sensory nerve damage prevents pain signals from reaching the brain.
2. Can neuropathic ulcers heal completely?
Yes, with proper offloading, wound care, and infection control, healing is possible.
3. Are neuropathic ulcers always related to diabetes?
No, but diabetes is the most common cause.
4. What is the earliest sign of a neuropathic ulcer?
Callus formation or skin discoloration at pressure points.
5. How can neuropathic ulcers be prevented?
Daily foot checks, good footwear, blood sugar control, and regular medical follow-up.


