Introduction
Foot wounds can be stubborn, slow to heal, and downright dangerous if ignored. Whether it’s a diabetic foot ulcer, an infected cut, or a pressure sore, one treatment often makes the biggest difference between healing and worsening. Debridement of foot is a cornerstone of modern wound management. In simple terms, it means removing dead, damaged, or infected tissue from a foot wound so healthy tissue can heal properly. Although it may sound intimidating, this procedure is often the turning point between a wound that lingers for months and one that finally begins to close.
Foot wounds are common, especially among older adults, people with diabetes, and those with poor circulation. When dead tissue stays in a wound, it becomes a breeding ground for bacteria. As a result, healing slows down, infections spread, and complications increase. That’s where debridement of foot plays a decisive role.
What Is Foot Debridement?
Simple Definition
Foot debridement is a medical procedure where dead, damaged, or infected tissue is removed from a wound on the foot. The goal? To help healthy tissue grow and allow the wound to heal faster.
Why Debridement Is Essential for Wound Healing
Dead tissue is like a roadblock. It traps bacteria, prevents oxygen from reaching healthy cells, and slows healing. By removing it, debridement.
- Reduces infection risk
- Improves blood flow to the wound
- Speeds up tissue regeneration
Without debridement, many foot wounds simply won’t heal.
Why Foot Wounds Need Debridement
Dead Tissue and Infection
When tissue dies, bacteria throw a party. That’s when wounds start to smell, ooze, and worsen. Debridement shuts that party down.
Poor Circulation and Delayed Healing
Feet especially in diabetic patients—often suffer from poor circulation. Debridement removes barriers so limited blood flow can still do its job.
Common Conditions That Require Foot Debridement
Diabetic Foot Ulcers
These are the most common reason for foot debridement. Loss of sensation means wounds go unnoticed and worsen quickly.
Pressure Sores
Often seen in bedridden or immobile patients, pressure sores on the heel need regular debridement.
Traumatic Foot Wounds
Accidents, burns, or deep cuts can leave behind non-viable tissue that must be removed.
Post-Surgical Wounds
Sometimes surgical wounds don’t heal as planned and require debridement to restart healing.
Types of Foot Debridement
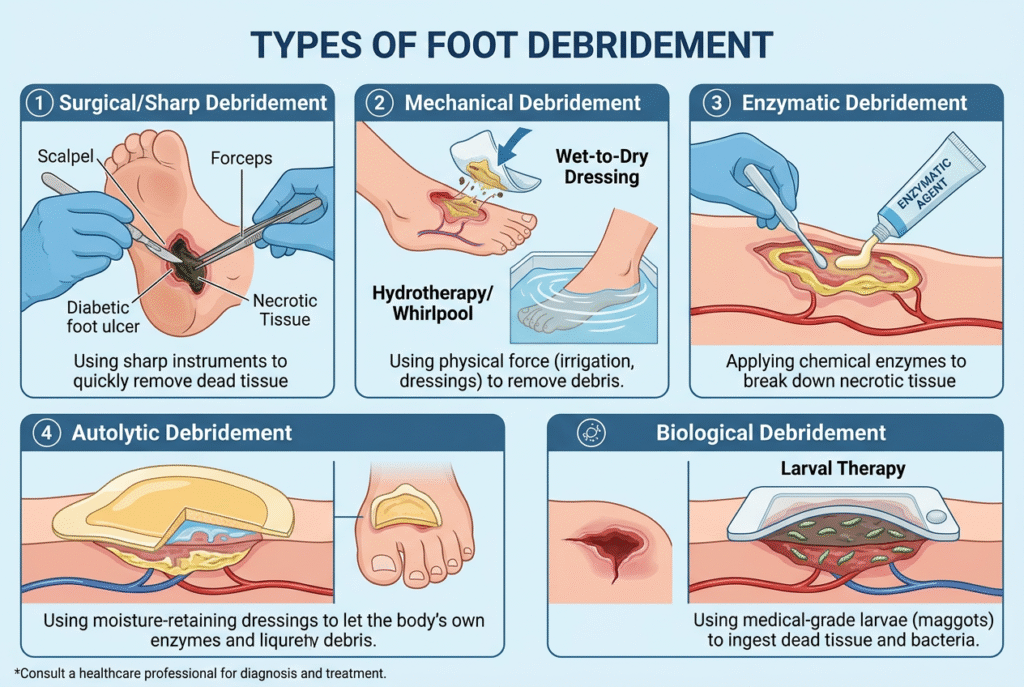
Surgical Debridement
This is the fastest and most precise method. A surgeon uses sterile instruments to cut away dead tissue. Surgical debridement of foot is ideal for severe infections or extensive necrosis.
- Pros: Immediate results, thorough cleaning
- Cons: Requires anesthesia, higher cost
Mechanical Debridement
Mechanical methods include wet-to-dry dressings or irrigation. As dressings are removed, dead tissue comes away with them.
- Pros: Simple, widely available
- Cons: Can be painful, may remove healthy tissue
Autolytic Debridement
This method lets the body do the work. Moist dressings encourage natural enzymes to break down dead tissue.
- Pros: Painless, selective
- Cons: Slower process
Enzymatic Debridement
Topical enzymes dissolve necrotic tissue without harming healthy cells.
- Pros: Effective for patients who can’t tolerate surgery
- Cons: Requires daily application
Biological (Maggot) Debridement
Sterile larvae selectively consume dead tissue. Though unconventional, it’s surprisingly effective.
- Pros: Highly selective, reduces bacteria
- Cons: Limited availability, patient hesitation
Surgical Debridement Explained
When It Is Needed
- Severe infection
- Rapidly spreading tissue damage
- High risk of amputation
How the Procedure Is Done
The area is cleaned, numbed (or anesthetized), and dead tissue is carefully cut away. It’s precise and controlled.
Non-Surgical Debridement Options
Who Is Eligible
Patients with mild to moderate wounds, minimal infection, or poor surgical tolerance.
Benefits and Limitations
These methods are gentler but slower. They often require patience and strict wound care.
Debridement of Foot in Diabetic Patients
Diabetes changes everything. Reduced sensation and poor circulation mean wounds go unnoticed and heal slowly.
Neuropathy and Poor Circulation
Because diabetic patients may not feel pain, minor injuries worsen quickly. Debridement of foot removes infected tissue before it spreads.
Preventing Amputation
Regular debridement of foot significantly lowers amputation risk. Studies consistently show better outcomes when dead tissue is removed early and repeatedly as needed.
Preparation Before Foot Debridement
Clinical Evaluation
Doctors assess:
- Blood flow
- Infection level
- Wound depth
Pain Management and Anesthesia
Pain varies by method. Surgical debridement of foot may require local or regional anesthesia. Autolytic and enzymatic methods are usually painless. Doctors always aim to keep patients comfortable.
Step-by-Step Procedure of Debridement of Foot
- Wound assessment and documentation
- Pain control or anesthesia
- Sterile preparation
- Removal of dead tissue
- Bleeding control
- Application of dressings
- Post-procedure care plan
Aftercare Following Foot Debridement
Dressing and Wound Care
Proper dressing keeps the wound moist but protected.
Infection Prevention
Antibiotics may be prescribed. Cleanliness is non-negotiable.
Healing Timeline After Debridement
What to Expect Week by Week
- Week 1: Reduced odor and infection
- Week 2–3: Granulation tissue forms
- Week 4+: Wound contracts and closes
Risks and Complications of Debridement of Foot
Like any medical procedure, risks exist:
- Bleeding
- Temporary pain
- Infection (rare when done properly)
- Damage to healthy tissue
However, the risks of not performing debridement of foot are far greater.
Post-Debridement Foot Care and Recovery
After debridement of foot, proper care is essential:
- Keep dressings clean and dry
- Avoid pressure on the wound
- Control blood sugar levels
- Attend follow-up visits
When to See a Doctor Immediately
Warning Signs You Should Never Ignore
- Increasing pain
- Fever
- Foul-smelling discharge
- Blackening of tissue
Future of Wound Care and Debridement
Precision-driven, technology-integrated, and regenerative approaches are replacing traditional, reactive management in the wound care industry. This development is especially important for chronic wounds like pressure injuries, diabetic foot ulcers, and venous leg ulcers.
Advanced Technologies
Laser debridement, bioengineered dressings, and smart wound monitoring are changing outcomes fast.
Conclusion
Debridement of the foot isn’t just a procedure—it’s a lifesaving step in wound care. By removing dead tissue, it gives your body a real chance to heal, prevents serious infections, and often saves limbs. Whether you’re a patient, caregiver, or clinician, understanding debridement empowers you to act early and wisely. Healthy healing always starts with a clean foundation.
FAQs
1. Is foot debridement painful?
Most patients feel minimal pain due to anesthesia or numbing agents.
2. How often is foot debridement needed?
It depends on the wound. Some need weekly sessions, others just once.
3. Can foot debridement be done at home?
Only very mild forms under medical guidance. Never attempt sharp debridement yourself.
4. How long does a wound take to heal after debridement?
Anywhere from weeks to months, depending on health and wound severity.
5. Does debridement prevent amputation?
In many cases, yes. Early and proper debridement significantly reduces amputation risk.

